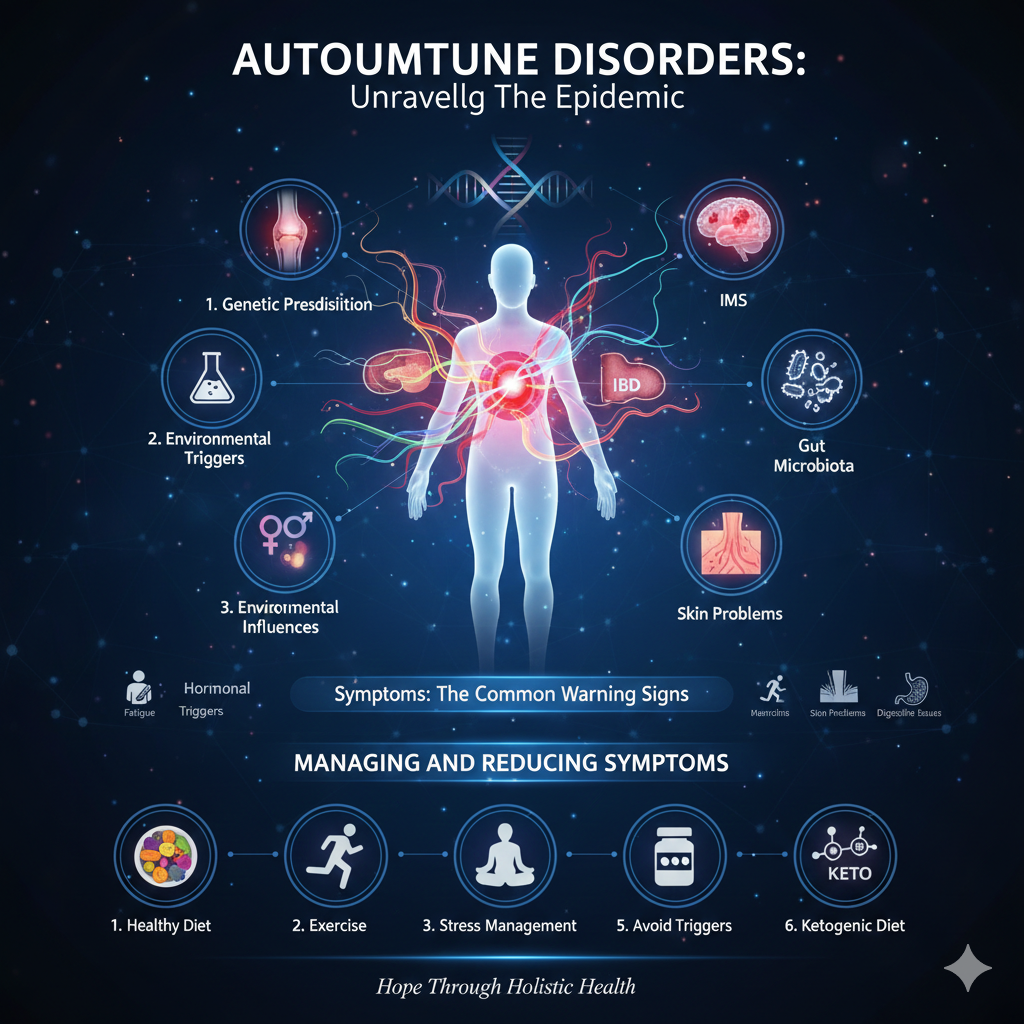
Autoimmune disorders are on the rise, quietly affecting millions worldwide. These complex conditions occur when the immune system—normally the body’s defense against invaders—mistakenly attacks its own healthy tissues. The result can range from chronic fatigue and joint pain to neurological symptoms and digestive distress. Let’s explore what causes autoimmune disorders, recognize the signs, and look at practical steps for living well—even in the face of this silent epidemic.
What Causes Autoimmune Disorders?
While no single trigger is responsible, most cases result from a combination of these factors:
Genetic Predisposition:
Certain genes make some individuals more vulnerable, especially those involving the HLA region—strongly linked to conditions like type 1 diabetes and multiple sclerosis.Environmental Triggers:
Viral infections, chemical exposures, and even aspects of the modern diet can trigger autoimmunity in genetically susceptible people.Hormonal Influences:
Autoimmune diseases disproportionately affect women, with hormones like estrogen and changes during puberty, pregnancy, or menopause playing a major role.Gut Microbiota:
An imbalanced gut—dysbiosis—can disrupt immune regulation, fueling conditions such as rheumatoid arthritis and inflammatory bowel disease.
Why Are Autoimmune Disorders Becoming More Common?
Better Diagnostics: Newer tests mean more people are properly diagnosed, which partly explains the increase.
Modern Lifestyles: Processed foods, environmental toxins, and higher exposure to chemicals may all contribute.
Hygiene Hypothesis: Lack of early microbial exposures may leave the immune system untrained, increasing autoimmune risk.
Chronic Stress: Elevated stress hormones disrupt immune function, raising the likelihood of autoimmunity.
Symptoms: The Common Warning Signs
Autoimmune symptoms are diverse and can include:
Fatigue (unexplained, persistent tiredness)
Joint pain and swelling
Skin problems (rashes, lesions)
Digestive issues (pain, diarrhea)
Recurring fevers
Swollen glands
Neurological changes (numbness, tingling, vision loss)
Managing and Reducing Autoimmune Symptoms
A multipronged approach often yields the best results:
Medications: Immunosuppressive and anti-inflammatory drugs control flare-ups.
Healthy Diet: Emphasize proteins and colorful produce, avoid ultra-processed foods, and minimize added sugars.
Exercise: Gentle, regular movement can reduce inflammation and boost mood.
Stress Management: Techniques like meditation, prayer, good sleep, and mindful breathing tame harmful stress responses.
Avoid Triggers: Identify (and minimize) foods, chemicals, or environments that worsen symptoms.
The Ketogenic Diet & Autoimmune Relief
The ketogenic diet—very low in carbs, higher in fat—has garnered interest for managing autoimmune symptoms:
Reduced Inflammation: Ketones act as anti-inflammatory agents, countering chronic inflammation common in autoimmunity.
Better Mitochondrial Function: Improvements in energy production may combat fatigue and brain fog.
Immune Modulation: By supporting a balanced immune response, keto can limit the overactivity seen in autoimmune flare-ups.
Proceed with caution: Consult your healthcare provider before major dietary changes, especially if you have other health issues or are on immune-modulating drugs.
Conclusion
Autoimmune disorders are complex—part genetics, part environment, and part lifestyle. But a holistic approach matters. Optimizing diet, managing stress, and working closely with your medical team can help you reduce symptoms and reclaim your quality of life. While a cure remains elusive, steady advances in nutrition, wellness, and medicine mean living well with autoimmunity is more possible than ever before.
References
- Ercolini, A. M., & Miller, S. D. (2009). The role of infections in autoimmune disease. Clinical and Experimental Immunology, 155(1), 1-15.
- Willison, H. J., Jacobs, B. C., & van Doorn, P. A. (2016). Guillain-Barré syndrome. The Lancet, 388(10045), 717-727.
- Hughes, G. C. (2012). Progesterone and autoimmune disease. Autoimmunity Reviews, 11(6-7), A502-A514.
- Belkaid, Y., & Hand, T. W. (2014). Role of the microbiota in immunity and inflammation. Cell, 157(1), 121-141.
- Cooper, G. S., & Stroehla, B. C. (2003). The epidemiology of autoimmune diseases. Autoimmunity Reviews, 2(3), 119-125.
- Bach, J. F. (2002). The effect of infections on susceptibility to autoimmune and allergic diseases. New England Journal of Medicine, 347(12), 911-920.
- Stojanovich, L., & Marisavljevich, D. (2008). Stress as a trigger of autoimmune disease. Autoimmunity Reviews, 7(3), 209-213.
- Davidson, A., & Diamond, B. (2001). Autoimmune diseases. New England Journal of Medicine, 345(5), 340-350.
- Paoli, A., Rubini, A., Volek, J. S., & Grimaldi, K. A. (2013). Beyond weight loss: a review of the therapeutic uses of very-low-carbohydrate (ketogenic) diets. European Journal of Clinical Nutrition, 67(8), 789-796.
- Volek, J. S., & Phinney, S. D. (2012). The Art and Science of Low Carbohydrate Living. Beyond Obesity LLC.
- Seyfried, T. N., & Mukherjee, P. (2005). Targeting energy metabolism in brain cancer: review and hypothesis. Nutrition & Metabolism, 2(1), 30.
- Fukui, M., Kitagawa, Y., Nakamura, N., Kadono, M., Mogami, S., Hirata, C., … & Miyao, M. (2000). Association between serum C-reactive protein concentration and carotid artery intima-media wall thickness in Japanese men. Atherosclerosis, 151(2), 511-516.
- Recent Post



One Response